Protocol - Visual Acuity
Description
Measurement of clarity or sharpness of vision (visual acuity) using the Early Treatment Diabetic Retinopathy Study (ETDRS) charts.
Specific Instructions
None
Availability
This protocol is freely available; permission not required for use.
Protocol
Early Treatment Diabetic Retinopathy Study (ETDRS) Visual Acuity Chart: Modified Bailey-Lovie
The ETDRS Refraction Chart R or any other visual acuity chart except ETDRS Visual Acuity Chart 1 or 2 many be used to determine the best distance lens correction, at 10 to 20 feet, for each eye. Testing of all patients, regardless of visual acuity, begins at four meters. Two ETDRS Visual Acuity Charts are used for the measurement of visual acuity, each with a different letter sequence. The right eye will always be tested with Chart 1 and the left eye with Chart 2.
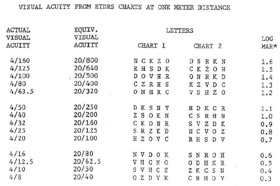
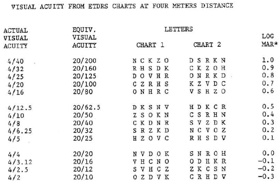
Visual acuity measured at four meters (and at one meter for low vision patents) may be determined from ETDRS Visual Acuity Charts as shown for Charts 1 and 2 in Table 1. The visual acuity equivalents for 20 feet are indicated. Visual acuity measured at one meter may be determined as shown in Table 2.
ETDRS Charts will be changed as needed to maintain high contrast letters on a white background. ETDRS Charts can be cleaned with a mild soap and water.
Illumination of the ETDRS Visual Acuity Charts and Room Illumination
The standard ETDRS chart light box is used at the four- and one-meter test distances. The fluorescent tubes in the ETDRS chart light box are to be 40 watt frosted cool white bulbs and are to be replaced annually each July 1. A record of the date changed and name of the individual who changed the bulb should be taped onto fixture. Room illumination should be at a level of 50 to 100 foot-candles as measured with a photometer held four feet from the floor and directed toward the ceiling. This is equivalent to the room lighting in most office buildings or schools. Illumination should be within the stated limits at all points along a line from the patient to the chart except for the three-foot segment closest to the chart, where the limit may be exceeded.
Best-Corrected Visual Acuity Measurements
The distance from the patients eyes to the ETDRS Visual Acuity Chart should be 4.0 meters. With the lens correction obtained by subjective refraction in the trial frame, the patient is asked to read ETDRS Visual Acuity Chart 1 from the top with the right eye. It is emphasized to the patient that each answer will be scored so that adequate time should be allowed for each letter in order to achieve the best identification.
When the patient cannot read a letter, he/she is encouraged to guess if at all possible. If the patient states that a letter is one of two letters, he/she is asked to choose only one letter and, if necessary, to guess. It may be suggested that the patient fixate eccentrically or turn or shake his/her head in any manner if this improves visual acuity. If the patent employs these maneuvers, care must be taken to insure that the fellow eye remains covered. Only one reading is allowed for each letter. When a patient attempts to read the chart and comes to a level at which he/she cannot even guess, the examiner may stop the test for that eye provided that the patient has previously made some errors which indicate that the best possible acuity level has been reached.
The examiner records each letter identified correctly by the patient as he/she reads the chart. Letters read incorrectly, or for which no guessed are made, are not recorded. Each letter read correctly is scored as one point. The score for each line (including zero if no letters were read correctly on that line) and the total score for the eye must be recorded after the testing has been completed.
If the number of letters read correctly at four meters is less than twenty, the test should be repeated at one meter and both the four- and one-meter totals should be recorded. Both eyes should be tested at four meters before the patient is moved up to the one-meter test distance. Prior to actual testing at one-meter, +0.75 spheres should be added to the correction already in the trial frame to compensate for the new distance. The patient may stand or sit for the visual acuity test at four meters, but must sit for the one-meter distance.
If the patients visual acuity is so poor that he/she cannot read the largest chart letters when tested at one meter (i.e., the number of letters read correctly at one meter is zero) then the patients ability to count fingers, detect hand motion, or have light perception should be evaluated. If the examiner is not convinced that the patient can count fingers or detect hand movements, this eye should be tested for light perception.
The same procedure for obtaining visual acuity for the right eye is used for the left eye, except that ETDRS Visual Acuity Chart 2 is used.
Calculating the Visual Acuity Score
After each measurement of visual acuity, the visual acuity score for the visit is calculated. The visual acuity score is defined as follows:
a. if four or more letters are read correctly at the four-meter test distance, the visual acuity score is equal to the number of letters read correctly at four meters plus 30; or
b. If fewer than four letters are read correctly at the four-meter test distance, the visual acuity score is equal to the number of letters read correctly at one meter; or
c. if no letters are read correctly at either the four-meter distance or the one-meter distance, the visual acuity score is 0.
Proposal for Conversion from Visual Acuity Examination Record Form to Visual Acuity Value
One may obtain a "fractional" visual acuity by noting the last full line read correctly and adding to it the number of letters read correctly beyond this line; for example, if a patient were to read all the letters on the 4/10 line and above and four of five letters on the 4/8 line, the acuity could be expressed as 4/10 + 4 (20/50 +4).
For purposes of statistical analyses, conversion to Log MAR units may be done. Each line of letters has a corresponding Log MAR value. It is assumed that each letter on the chart has a Log MAR value of 0.02, as each line of five letters has a total value of 0.10. One may therefore arrive at a Log MAR value for each test by the calculation (1.70 0.02 N) where N is the total number of letters read correctly. For patients tested at the four-meter test distance, 30 letters will be considered as having been read correctly prior to testing, in order to have scores attained at four meters and one meter correspond. In the example, by this method, N= (30+39) = 69 and the Log MAR value would be 1.70 (0.02 x 69) = 0.32. In other words, it is assumed, for scoring purposes, that the patient could read the 30 largest letters at one meter without actually testing this ability.
It should be noted that this method of conversion to Log MAR units has the difficulty of assigning the same 0.02 value to each letter read correctly, no matter which line the letter is from. Therefore, any letter on the 4/6.25 (20/32) line is given the same 0.02 value as any letter on the 4/8 (20/40) line, or any other line for that matter. While some accuracy may be lost by this method, the error is estimated to be small and the advantage of giving some credit for all correct answers probably outweighs this disadvantage.
Below are examples of ETDRS Visual Acuity Charts 1 and 2.
Table 1
Table 2
Personnel and Training Required
Certified visual acuity examiner
Equipment Needs
Early Treatment Diabetic Retinopathy Study (ETDRS) visual acuity charts 1 and 2
Requirements
| Requirement Category | Required |
|---|---|
| Major equipment | No |
| Specialized training | No |
| Specialized requirements for biospecimen collection | No |
| Average time of greater than 15 minutes in an unaffected individual | No |
Mode of Administration
Clinical Measurement
Lifestage
Child, Adolescent, Adult
Participants
Adults aged 18 to 70 years*
* While the source of this protocol was a study of adults aged 18 to 70 years, the Ocular Working Group notes that this protocol has reliably been used with individuals aged 5 years and older (see "General References" for study citations).
Selection Rationale
The Early Treatment Diabetic Retinopathy Study (ETDRS) chart is the standard for ophthalmic research. The ETDRS test incorporates specific design criteria that have proven accuracy.
Language
English
Standards
| Standard | Name | ID | Source |
|---|---|---|---|
| Logical Observation Identifiers Names and Codes (LOINC) | Visual acuity proto | 62698-6 | LOINC |
| Human Phenotype Ontology | Reduced visual acuity | HP:0007663 | HPO |
| Human Phenotype Ontology | Visual acuity test abnormality | HP:0030532 | HPO |
| caDSR Form | PhenX PX111101 - Visual Acuity | 5973247 | caDSR Form |
Derived Variables
None
Process and Review
Not applicable.
Protocol Name from Source
National Eye Institute (NEI), Early Treatment Diabetic Retinopathy Study (ETDRS), 1979-1989
Source
National Eye Institute, Early Treatment Diabetic Retinopathy Study (ETDRS), 1979-1989.
ETDRS Manual of Operations, Chapter 12 Procedures for completing eye examinations, section 12.2 Best-corrected Visual Acuity Measurements
Ferris FL 3rd, Kassoff A, Bresnick GH, Bailey I. (1982). New visual acuity charts for clinical research. Am J Ophthalmol, 94(1):91-6.
General References
Manny RE, Hussein M, Gwiazda J, Marsh-Tootle W; COMET Study Group. (2003). Repeatability of ETDRS visual acuity in children. Invest Ophthalmol Vis Sci, 44(8):3294-300.
Dobson V, Clifford-Donaldson CE, Green TK, Miller JM, Harvey EM. (2009). Normative monocular visual acuity for early treatment diabetic retinopathy study charts in emmetropic children 5 to 12 years of age. Ophthalmology, 116(7):1397-401.
Protocol ID
111101
Variables
Export Variables| Variable Name | Variable ID | Variable Description | dbGaP Mapping | |
|---|---|---|---|---|
| PX111101_Actual_Visual_Acuity_Left_Eye | ||||
| PX111101080000 | Actual visual acuity is the measured visual more | Variable Mapping | ||
| PX111101_Actual_Visual_Acuity_Right_Eye | ||||
| PX111101030000 | Actual visual acuity is the measured visual more | Variable Mapping | ||
| PX111101_Equivalent_Visual_Acuity_Left_Eye | ||||
| PX111101090000 | The equivalent visual acuity from table more | N/A | ||
| PX111101_Equivalent_Visual_Acuity_Right_Eye | ||||
| PX111101040000 | The equivalent visual acuity from table more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line1 | ||||
| PX111101070100 | The letter on line 1 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line10 | ||||
| PX111101071000 | The letter on line 10 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line11 | ||||
| PX111101071100 | The letter on line 11 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line12 | ||||
| PX111101071200 | The letter on line 12 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line13 | ||||
| PX111101071300 | The letter on line 13 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line14 | ||||
| PX111101071400 | The letter on line 14 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line2 | ||||
| PX111101070200 | The letter on line 2 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line3 | ||||
| PX111101070300 | The letter on line 3 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line4 | ||||
| PX111101070400 | The letter on line 4 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line5 | ||||
| PX111101070500 | The letter on line 5 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line6 | ||||
| PX111101070600 | The letter on line 6 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line7 | ||||
| PX111101070700 | The letter on line 7 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line8 | ||||
| PX111101070800 | The letter on line 8 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Letter_Line9 | ||||
| PX111101070900 | The letter on line 9 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_LeftEye_Testing_Distance | ||||
| PX111101060000 | The distance from the patient's eyes to the more | N/A | ||
| PX111101_Visual_Acuity_LogMAR_Left_Eye | ||||
| PX111101100000 | The visual acuity LogMAR value converted more | N/A | ||
| PX111101_Visual_Acuity_LogMAR_Right_Eye | ||||
| PX111101050000 | The visual acuity LogMAR value converted more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line1 | ||||
| PX111101020100 | The letter on line 1 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line10 | ||||
| PX111101021000 | The letter on line 10 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line11 | ||||
| PX111101021100 | The letter on line 11 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line12 | ||||
| PX111101021200 | The letter on line 12 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line13 | ||||
| PX111101021300 | The letter on line 13 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line14 | ||||
| PX111101021400 | The letter on line 14 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line2 | ||||
| PX111101020200 | The letter on line 2 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line3 | ||||
| PX111101020300 | The letter on line 3 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line4 | ||||
| PX111101020400 | The letter on line 4 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line5 | ||||
| PX111101020500 | The letter on line 5 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line6 | ||||
| PX111101020600 | The letter on line 6 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line7 | ||||
| PX111101020700 | The letter on line 7 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line8 | ||||
| PX111101020800 | The letter on line 8 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Letter_Line9 | ||||
| PX111101020900 | The letter on line 9 in the ETDRS Visual more | N/A | ||
| PX111101_Visual_Acuity_RightEye_Testing_Distance | ||||
| PX111101010000 | The distance from the patient's eyes to the more | N/A | ||