Protocol - Body Composition - Subscapular Skinfold Thickness
- Hip Circumference - Hip Circumference
- Waist Circumference - Framingham Heart Study
- Waist Circumference - Waist Circumference NCFS
- Waist Circumference - Waist Circumference NHANES
- Current Age
- Ethnicity and Race
- Height - Knee Height
- Height - Recumbent Length
- Height - Self-Reported Height
- Height - Standing Height
- Weight - Measured Weight
- Weight - Self-Reported Weight
Description
Measurement of the study subject subcutaneous fat mass using calipers to measure skinfold thickness at the subscapular. Skinfold thicknesses may also be measured at a number of other sites, including the midaxillary, pectoral, abdominal, anterior thigh, suprapatellar, medial calf, biceps, and forearm sites. If these latter sites are of interest, definitions and protocols are available in manuals that describe anthropometric measurements.
Specific Instructions
There are several overarching, critical issues for high-quality data collection of anthropometric measures that optimize the data in gene-environment etiologic research. These issues include: (1) the need for training (and re-training) of study staff in anthropometric data collection; (2) duplicate collection of measurements, especially under field conditions; (3) use of more than one person for proper collection of measurements where required; (4) accurate recording of the protocols and the measurement units of data collection; and (5) use of required and properly calibrated equipment.
The notion of recommending replicate measurements comes from the reduction in random errors of measurement and accompanying improved measurement reliability when the mean of multiple measurements is used rather than the a single measurement. This improvement in measurement reliability, however, depends upon the reliability of a single measurement in the hands of the data collectors in a particular study (Himes, 1989). For example, if a measure like recumbent length in a given study has a measurement reliability of 0.95 (expressed as an intraclass correlation coefficient), taking a second measurement and using the mean of the two in analyses will only improve the reliability to 0.97, yielding only a 2% reduction in error variance for the additional effort. If in the same study, the reliability of a single triceps skinfold measurement was 0.85, using the mean including a replicate measurement would raise the reliability to 0.92 and yield a 7% reduction in error variance, more than a threefold improvement compared with recumbent length.
Because the benefits of taking replicate measurements are so closely linked with the existing measurement reliability, it is recommended that as a part of the training of those who will be collecting anthropometry data, a reliability study be conducted that will yield measurement reliability estimates for the data collectors, protocols, settings and participants involved in that particular study (Himes, 1989). If the measurement reliability for a single measurement ≥ 0.95 the recommendation is that replicate measurements are not necessary and will yield little practical benefit. If the measurement reliability <0.95, the recommendation is to include replicate measurements as prescribed.
If replicate measurements are indicated because of relatively low reliability, a second measurement should be taken, including repositioning the participant. A third measurement should be taken if the first two measurements differ by >2.0 mm. If it is necessary to take a third measurement, the two closest measurements are averaged. If the third measurement falls equally between the first two measurements, all three should be averaged.
The Expert Review Panel notes that measurements should be made at the precision levels of the calipers chosen (dial graduation mark). Suggestions for acceptable calipers and their precision are given below.
Availability
This protocol is freely available; permission not required for use.
Protocol
Subscapular Skinfold: The subscapular skinfold is measured at the inferior angle of the right scapula. Instructions for performing the subscapular skinfold measure are provided below:
1. Position the participant: Similar to the triceps skinfold measure, turn the participant so that you stand behind his or her right side. Have the participant stand upright with weight evenly distributed on both feet, shoulders relaxed, and arms hanging loosely at the sides.
2. Mark the measurement site: Tell the participant that you are going to open the gown in the back and mark the skin with the cosmetic pencil. Open the back of the gown and palpate for the inferior angle, or triangle portion, of the right scapula (Exhibit 6). Using the cosmetic pencil, mark a cross (X) on the inferior angle (Exhibit 7). Make the first line at 45º to the spine and cross this with a line that bisects the inferior angle of the scapula.
3. Grasp the skinfold: Using your thumb and index finger, grasp a fold so that the index finger remains situated roughly 2.0 cm above and medial to the inferior angle of the scapula. Due to tightness in this area of the back on many participants, obtaining this skinfold measure can be a challenge. In the cases where you experience difficulty separating the subscapular skinfold from the underlying tissue, begin grasping the fold with the thumb and index finger spread wide.
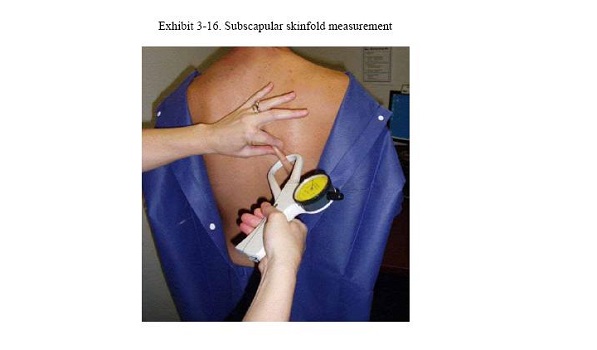
4. Position the caliper: Continue to hold the skinfold in place. With the other hand, set the top jaw of the caliper on the "+" mark. This differs from the triceps skinfold procedure in which the mark is centered between the caliper tips. Position the tips of the caliper jaws over the complete skinfold perpendicular to the length of the fold and roughly 2.0 cm lateral to the fingers (Exhibit 8).
5. Take the measurement: Continue to hold the skinfold in place and release the caliper handle to exert full tension on the skinfold. Wait 3 seconds for the needle on the caliper dial to settle on an accurate measurement. Read the thickness to the nearest 0.2 mm.
6. Record the result. Remove the caliper jaws first and then let go of the skinfold.
Exhibit 6. Location of subscapular skinfold Exhibit 7. Subscapular skinfold mark
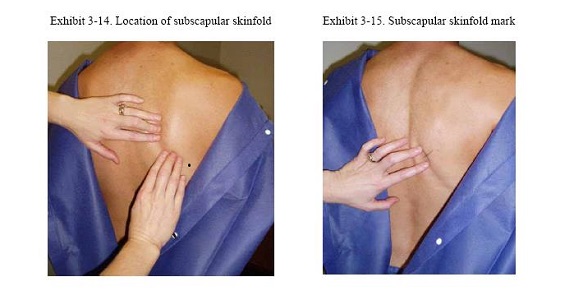
Exhibit 8. Subscapular skinfold measurement
Personnel and Training Required
Trained to use skinfold calipers, National Health and Nutrition Examination Survey (NHANES) training video available at: http://www.cdc.gov/nchs/nhanes/nhanes3/anthropometric_videos.htm.
Equipment Needs
Skinfold caliper, the type of caliper used should be recorded. A table of commonly used skinfold calipers appears below.
| Caliper | Measuring range | Dial graduation | Measuring pressure | |
| Harpenden Skinfold Caliper | [img[020304_Body_Composition_Triceps_3.jpg|]] | 0 to 80 mm | 0.2 mm, accurate to 0.2 mm | 10 g/mm2 |
| Lange Skinfold Caliper | [img[020304_Body_Composition_Triceps_4.jpg|]] | 0 to 60 mm | 1.0 mm, accurate to 0.5 mm | 10 g/mm2 |
| Holtain Tanner/Whitehouse Skinfold Caliper | [img[020304_Body_Composition_Triceps_5.jpg|]] | 0 to 46 mm | 0.2 mm, accurate to 0.2 mm | 10 g/mm2 |
Requirements
| Requirement Category | Required |
|---|---|
| Major equipment | No |
| Specialized training | No |
| Specialized requirements for biospecimen collection | No |
| Average time of greater than 15 minutes in an unaffected individual | No |
Mode of Administration
Physical Measurement
Lifestage
Infant, Toddler, Child, Adolescent, Adult, Senior
Participants
Participants at all ages, including neonates
Selection Rationale
Throughout all of the cycles where skinfolds were collected, National Health and Nutrition Examination Survey (NHANES) kept to a rigorous training and reliability schedule for their anthropometrists, and the NHANES protocols are consistent with best practices in the field. Skinfold-based measures of fatness and fat distribution in children and adults have been consistently found to agree better with fatness and fat distribution measured by dual-energy x-ray absorptiometry (DXA) than other commonly used indices of body composition, e.g., body mass index (BMI) and waist-to-hip ratio (WHR), that are collected in field situations.
Language
English
Standards
| Standard | Name | ID | Source |
|---|---|---|---|
| Human Phenotype Ontology | Abnormality of subcutaneous fat tissue | HP:0001001 | HPO |
| caDSR Form | PhenX PX020304 - Body Composition Subscapular Skinfold Thickness | 5801686 | caDSR Form |
Derived Variables
Centripetal fat ratio (CFR)
Process and Review
The Expert Review Panel #1 reviewed the measures in the Anthropometrics, Diabetes, Physical Activity and Physical Fitness, and Nutrition and Dietary Supplements domains.
Guidance from the ERP includes:
a. Added a new protocol
b. New Data Dictionary
Protocol Name from Source
National Health and Nutrition Examination Survey (NHANES), Anthropometry Procedures Manual, 2007
Source
Centers for Disease Control and Prevention (CDC), National Center for Health Statistics (NCHS). (2007). National Health and Nutrition Examination Survey 2007-2008 Anthropometry Procedures Manual. Retrieved from http://www.cdc.gov/nchs/data/nhanes/nhanes_07_08/manual_an.pdf
General References
Addo, O. Y., & Himes, J. H. (2014). Are field measures of adiposity sufficient to establish fatness-related linkages with metabolic outcomes in adolescents. Eur J Clin Nutr, 68(6), 671-676. doi: 10.1038/ejcn.2014.14
Addo, O. Y., Pereira, M. A., & Himes, J. H. (2012). Is skinfold thickness as good as DXA when measuring adiposity contributions to insulin resistance in adolescents? Amer J Hum Bio, 24(6), 806-811. doi: 10.1002/ajhb.22321
Fosbol, M., & Zehran, B. (2014). Contemporary methods of body composition measurement. Clinical Physiology and Functional Imaging, 35(2), 81-97. doi:1111/cpf.12152.
Himes, J. H. (1989). Reliability of anthropometric methods and replicate measurements. American Journal of Physical Anthropology, 79(1), 77-80.
Ketel, I. J. G., Volman, M. N. M., Seidell, J. C., Stehouwer, C. D. A., Twisk, J. W., & Lambalk, C. B. (2007). Superiority of skinfold measurements and waist over waist-to-hip ratio for determination of body fat distribution in a population-based cohort of Caucasian Dutch adults. Eur J Endocr, 156(6), 655-661. doi: 10.1530/eje-06-0730
Lohman, T. G., Roche, A. F., & Martorell, R. (1988). Anthropometric standardization reference manual (31, pp. 1493-1494). Champaign, IL, Human Kinetics Books.
Ward, L. C., Poston, L., Godfrey, K. M., & Koletzko, B. (2013). Assessing early growth and adiposity: Report from an Early Nutrition Academy workshop. Annals of Nutrition and Metabolism, 63(1-2), 120-130. doi:10.1159/000350702
Wang, J., Thornton, J. C., Kolesnik, S., Pierson, R. N., Jr. (2000). Anthropometry in body composition. An overview. Annals of the New York Academy of Science, 904, 317-326.
Wells, J. C. K. (2014). Toward Body Composition Reference Data for Infants, Children, and Adolescents. Advances in Nutrition: An International Review Journal, 5(3), 320S-329S. doi: 10.3945/an.113.005371
Wohlfahrt-Veje, C., Tinggaard, J., Winther, K., Mouritsen, A., Hagen, C. P., Mieritz, M. G., . . . Main, K. M. (2014). Body fat throughout childhood in 2647 healthy Danish children: agreement of BMI, waist circumference, skinfolds with dual X-ray absorptiometry. Eur J Clin Nutr, 68(6), 664-670. doi: 10.1038/ejcn.2013.282
Protocol ID
20304
Variables
Export Variables| Variable Name | Variable ID | Variable Description | dbGaP Mapping | |
|---|---|---|---|---|
| PX020304_BodyComposition_Subscapular_Adequate_Training | ||||
| PX020304030000 | Is the team adequately staffed so that more more | N/A | ||
| PX020304_BodyComposition_Subscapular_Caliper_Measurement | ||||
| PX020304100000 | When the caliper handle was released to more | N/A | ||
| PX020304_BodyComposition_Subscapular_Caliper_Orientation | ||||
| PX020304090000 | While holding the skinfold, were the tips of more | N/A | ||
| PX020304_BodyComposition_Subscapular_Cross_OnBack | ||||
| PX020304070000 | Using a cosmetic pencil, was a cross (X) more | N/A | ||
| PX020304_BodyComposition_Subscapular_Duplicate_Measurements | ||||
| PX020304020000 | Will duplicate measurements taken? | N/A | ||
| PX020304_BodyComposition_Subscapular_Measurement | ||||
| PX020304110000 | What was the measurement of the thickness of more | N/A | ||
| PX020304_BodyComposition_Subscapular_Proper_Equipment | ||||
| PX020304050000 | Has the staff been properly trained in the more | N/A | ||
| PX020304_BodyComposition_Subscapular_Quality_Training | ||||
| PX020304040000 | Has the staff been properly trained to more | N/A | ||
| PX020304_BodyComposition_Subscapular_SkinGrasp_Placement | ||||
| PX020304080000 | Was a fold of skin grasped using the thumb more | N/A | ||
| PX020304_BodyComposition_Subscapular_Subject_Instructions | ||||
| PX020304060000 | Was the participant instructed to stand more | N/A | ||
| PX020304_BodyComposition_Subscapular_Training | ||||
| PX020304010000 | Have the study staff undergone any training more | N/A | ||